Rotator cuff arthropathy
Print PdfAnterior Deltoid Program
Print PdfPatient Information Booklet Verso - Stemless Reverse Total Shoulder Replacement
VERSO - Stemless Reverse Total Shoulder Replacement
Rotator cuff tear arthropathy is a problem that occurs when a patient has both shoulder arthritis and an irreparable rotator cuff tear. This condition results in a weak and painful shoulder joint. When the rotator cuff is torn, the shoulder can wear out, leading to shoulder arthritis.
The shoulder is a ball and socket joint with a large range of movement. The joint sometimes needs replacing. This is usually when severe arthritis affects the joint surfaces and the shoulder becomes painful and difficult to move.
The rotator cuff is the group of tendons and muscles that surround the shoulder joint. These muscles and tendons are important in performing shoulder tasks (such as lifting your arm overhead), and keeping the ball of the ball-and-socket shoulder joint centered.
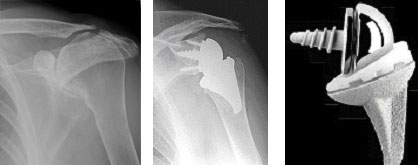
In a traditional shoulder replacement, the ball of the top of the arm bone (the humerus) is resurfaced or replaced with a metal ball. The socket of the shoulder blade (scapula) may be retained or replaced with a plastic socket. The absence of a rotator cuff causes the implant to move abnormally resulting in unusual forces on the artificial joint. This leads to a poor functional result and early failure of the replaced joint.
What is a reverse shoulder replacement?
The reverse shoulder replacement uses a ball-and-socket joint as well, but the ball is placed on the shoulder blade, and the socket is placed on top of the arm bone. This is the reverse of our normal anatomy, and thus the name "reverse shoulder replacement."
Why reverse the anatomy?
The reverse shoulder replacement is designed for patients who do not have a functioning rotator cuff, and therefore do not have "normal" shoulder anatomy. By reversing the ball and the socket, the large deltoid muscle which forms the contour of the shoulder becomes more efficient mechanically and is able to lift the arm up overhead, to compensate for the torn rotator cuff.
Are there problems with a reverse shoulder replacement?
Loosening of the implants, Fracture of the arm bone or socket, instability or dislocation of the ball from the socket, and persistent pain. Over time, the prosthesis could erode and damage bone stock.
What is the VERSO reverse shoulder replacement?
This is a special bone conserving reverse total shoulder replacement. It follows the basic principles of reverse replacements, but is bone preserving and causes less bone erosion over the longer period. It was developed at the Reading Shoulder Unit, over a period of 10 years. The prosthesis uses special coating called hydroxyapatite that allows the bone to bond onto the prosthesis over 12 weeks, thus avoiding the use of bone cement with its problems. It has a special screw-in base plate and ball for the shoulder blade, and a short finned socket for the top of the arm bone. It has been implanted in patients for 8 years with very promising early results.
Who is a good patient for a reverse shoulder replacement?
Patients interested in a reverse shoulder replacement must have significant pain from shoulder arthritis, and an irreparable rotator cuff tear or non-functioning rotator cuff muscles. Patients who do not have this combination of conditions can usually undergo other surgical procedures to address their problem.
The deltoid muscle should be functioning.
Patients interested in having this procedure should discuss all of their options with their orthopaedic surgeons. Certainly a reverse shoulder replacement should only be performed if simpler, non-operative treatments have failed to alleviate symptoms.
The Operation
The operation is performed under a general anaethetic with a nerve block. Sometimes, it is possible to perform the procedure under nerve block alone, especially in patients who may be a high risk for general anaesthetic.
The new reverse ball and socket joint is inserted sacrificing only a minimum quantity of bone to preserve as much good bone stock as possible in the event of future surgery.
General Advice
The operation lasts approximately 90 minutes. You will usually be in hospital for about 2 – 3 days after your operation. Following your surgery you will be in a sling. This is for comfort only and you may take it off as you wish.
A physiotherapist will see you in hospital to give you advice about using your arm and exercises. Outpatient physiotherapy will be arranged when you are discharged.
Your arm will be painful at first and in the first three to four weeks you will be quite one handed which will significantly affect your daily activities.
As your pain improves so will the amount you can use your arm.
Driving and most light activities are usually possible four to six weeks after the surgery. However the strength in your arm will take longer to improve, and will be dependent on the amount of pain and stiffness you had prior to the surgery.
A doctor or physiotherapist will discuss this with you.
Complications
As with all surgery there is a risk of some complications. These are rare, but you should be aware of them before your operation. They include:
- Complications relating to the anaesthetic.
- Infection
- Dislocation
- Fracture of the arm bone or the acromion
- Unwanted prolonged pain and/or stiffness
- Damage to the nerves or blood vessels around the shoulder.
- Loosening and Wear
- A need to redo the surgery.
- If you require further information please discuss with the doctors either in clinic or on admission.
What to expect
Following your operation you will have a scar approximately 3 inches (6-9 cm) long on the front of your shoulder.
Your arm will be supported in a sling and a physiotherapist will teach you how to take it on and off to do your exercises. You will be in hospital for about 2-3 days.
General guidelines
- Pain: A nerve block is usually used during the operation which means that immediately after the operation the shoulder and arm may feel numb. This may last a few hours. After this your shoulder will be painful and this may last a few weeks. You will be given painkillers to help this whilst in hospital. These should be continued after you are discharged home.
- Wearing a Sling: You will return from theatre wearing a sling. This is used for the first 3 weeks following your operation. It is important that you remove the sling to exercise. You can stop wearing the sling as soon as you feel comfortable.
- The Wound: Keep the wound dry until it is healed. This normally takes 10 to 14 days. Your stitch is dissolvable and needs only to be trimmed at your clinic visit.
- Driving: This is usually possible after about eight weeks, but will be dependant on your recovery.
- Returning to work: This is dependent upon your occupation. Light activities which involve using your arm in front of your body may be resumed after about three weeks. If you carry out heavy work, you may need to consider an alternative occupation.
- Leisure activities: Gentle swimming and exercises in water can begin at 4 to 6 weeks, Golf at 6 weeks.
- Follow up appointments: You will have an appointment to see the doctor/specialist physiotherapist three weeks after your operation.
- Progress: This is variable and dependant on the amount of movement and the strength of your muscles prior to surgery. Following discharge your pain will slowly decrease and you will become more confident. You will be able to use your arm in front of you for light activities. After six weeks your strength will start to improve.
- Exercises: You will start exercises on the first day after your operation. A physiotherapist will see you to teach you these and progress them. Out patient physiotherapy will be arranged for when you are discharged.
Verso Registry data collection forms:

